ABSTRACT
Limb Lengthening and Deformity Correction: A Practical Overview
Limb lengthening and deformity correction remain among the most demanding—and rewarding—areas of limb reconstruction. These procedures are technically complex and require long treatment timelines, yet they can restore alignment, function, and mobility when executed with careful planning and appropriate technique selection.
Recent literature highlights meaningful advances in preoperative planning, fixation strategies, and construct modulation, offering surgeons more precise and patient‑adapted solutions.[1][2][3]
Planning: From Manual Sketches to Digital Precision
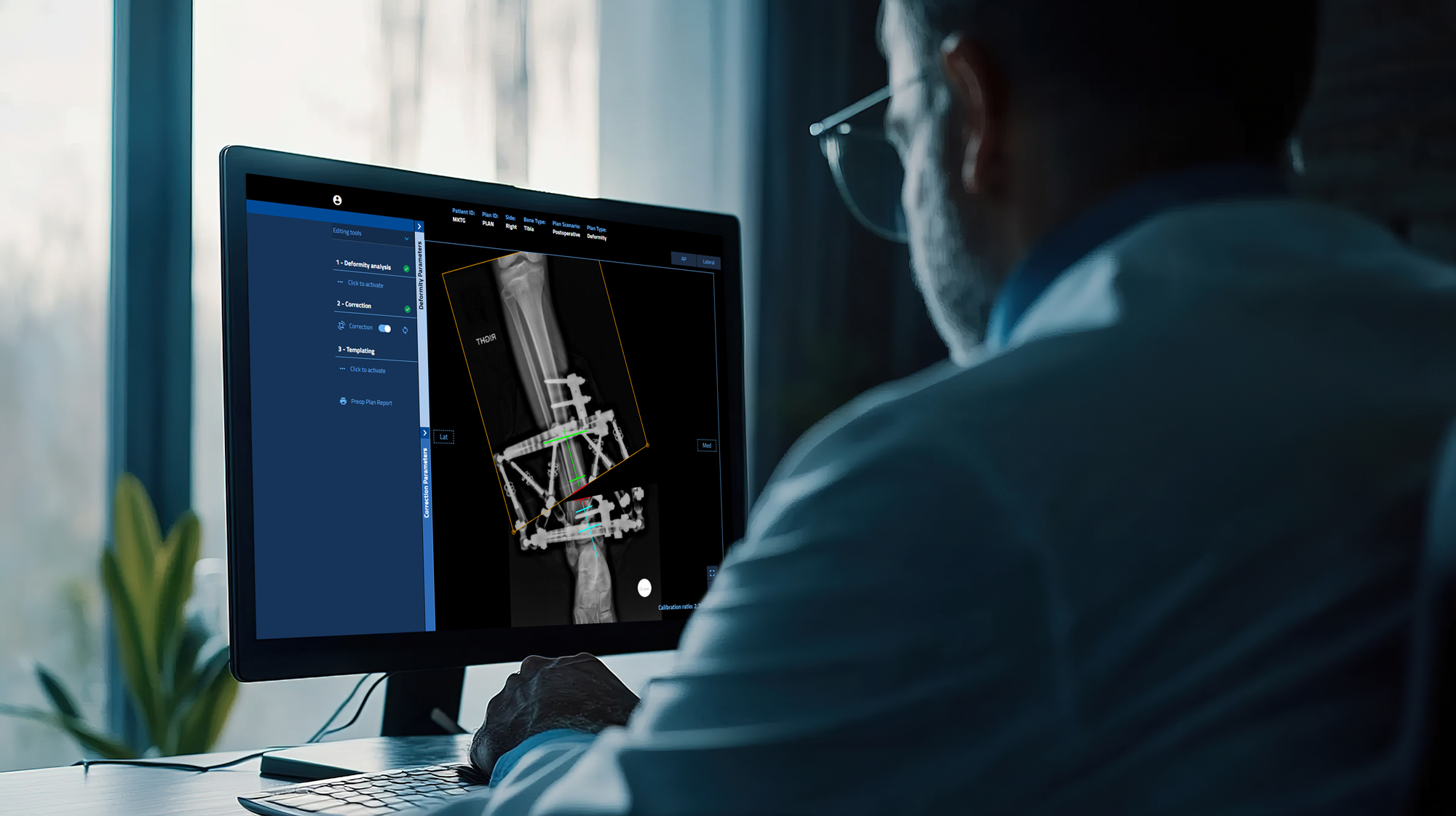
Historically, deformity planning relied on hand‑drawn diagrams, overlays, and fluoroscopic interpretation. Digital planning platforms such as Orthofix OrthoNext™ now enable more structured and reproducible workflows.[3][5][6][1]
Recent studies demonstrate that CT‑based and software‑assisted planning tools can accurately elaborate mechanical axes, joint orientation angles, and deformity vectors while substantially reducing planning time. Reports suggest a reduction from approximately one hour per case to less than 15 minutes, without compromising measurement accuracy.[1]
For surgeons managing complex limb lengthening and deformity correction cases, digital planning has become a practical expectation rather than an optional add‑on. While clinical judgment remains essential, software tools help streamline geometric analysis and improve consistency.[3][1]
Intramedullary Lengthening Nails
Motorized intramedullary lengthening nails have evolved from niche implants to widely adopted solutions, particularly in femoral lengthening. Clinical series show favorable bone‑healing indices, even when regenerate appearance on imaging appears irregular during distraction.[7][1]
These findings are clinically relevant, as radiographic irregularities do not necessarily predict regenerate failure, especially in well‑selected femoral cases. However, intramedullary techniques still require strict attention to indications, osteotomy technique, alignment control, and patient compliance.[8][4][1]
From the patient perspective, internal lengthening strategies reduce pin‑site care requirements and external frame–related skin complications. In suitable cases, a nail‑centered strategy—either fully internal or lengthening over nail—may simplify postoperative management while maintaining reconstructive effectiveness.[9][7] External fixation, however, remains the preferred approach in specific indications and anatomic settings.
Dynamization and Reverse Dynamization: Modulating Stability
Construct stiffness has emerged as a modifiable variable in distraction osteogenesis. Experimental models comparing static fixation, dynamic fixation, and reverse dynamization—initial stiffness followed by gradual loosening—have shown that reverse dynamization can accelerate regenerate formation and remodeling.[1][3]
These findings support the concept that controlled micro‑motion may stimulate callus maturation. In clinical practice, this does not translate into indiscriminate loosening but rather into structured dynamization protocols tailored to regenerate quality and consolidation progress.[4][8][3][1]
Stiffness should therefore be viewed as a tunable parameter. When regenerate progression appears delayed, thoughtful adjustment of construct rigidity can serve as an adjunctive strategy rather than a corrective measure of last resort.[3][1]
Key Takeaways for Clinical Practice
Recent advances in limb lengthening and deformity correction suggest several practical principles:
- Use digital planning tools to improve efficiency and consistency without replacing clinical reasoning[1][3]
- Incorporate intramedullary nails and hybrid strategies alongside external fixation when indicated[9][7]
- Consider construct stiffness as adjustable, using controlled dynamization to support regenerate maturation[3][1]
- Maintain focus on fundamentals, including osteotomy technique, patient selection, and early imaging assessment[4][5]
Despite technological progress, outcomes continue to depend on meticulous execution of core principles.
Conclusion
Modern limb lengthening and deformity correction benefit from improved planning systems, evolving fixation technologies, and a deeper understanding of biologic and mechanical interactions. While tools and techniques continue to advance, thoughtful integration of these options—guided by experience and patient‑specific factors—remains central to successful reconstruction.
References
- https://orthobuzz.jbjs.org/2024/08/22/whats-new-in-limb-lengthening-and-deformity-correction-2024/
- https://pubmed.ncbi.nlm.nih.gov/38896731/
- https://www.jbjs.org/reader.php?rsuite_id=455f8a71-57ff-40e8-8e93-5a5bb187ac8c
- https://www.science.gov/topicpages/i/ilizarov+limb+lengthening
- https://pmc.ncbi.nlm.nih.gov/articles/PMC2628228/
- https://www.jbjs.org/archive.php?j=jbjs&y=2023&v=105&i=16
- https://pmc.ncbi.nlm.nih.gov/articles/PMC12168351/
- https://worldwidescience.org/topicpages/i/ilizarov+limb+lengthening.html
- https://sciety.org/articles/activity/10.20944/preprints202506.0072.v1
 Home
Home About us
About us Educational Events
Educational Events Experience
Experience Resources Limb Reconstruction
Resources Limb Reconstruction Social Responsibility
Social Responsibility Contact us
Contact us Privacy policy
Privacy policy Cookie policy
Cookie policy